The rate can be 300 b/min, less or more (the latter in truly atypical atrial flutter). The P wave in lead V1 is usually negative. Thus paradoxically, some drugs used to slow the heart rate may in fact end up increasing it! This can have dangerous consequences.Ītypical atrial flutter ( Table 44.1) is a rare rhythm disturbance, recognized when the deflections in the inferior leads are positive (probably as the circuit proceeds in a clockwise rotation, rather than the anti-clockwise motion of typical atrial flutter). Sometimes anti-arrhythmic drugs (such as propafenone) can slow the atrial rate, say to 250 b/min, sufficient for the AV node to allow 1 to 1 conduction. If the rate of transmission is (in the absence of anti-arrhythmic drugs) less than this, say 1 in 5 or 1 in 6, then there is a high probability that there is also intrinsic conducting tissue disease. Sometimes the conduction is 1 in 3 or 4, giving a QRS rate respectively of 100 and 75 b/min. This has led to an aphorism in arrhythmology whenever a tachycardia is seen with a heart rate of exactly 150 b/min, the rhythm disturbance is atrial flutter until proved otherwise. This is too fast for the atrioventricular (AV) physiologically to allow for 1 to 1 conduction down to the ventricles, and usually a fixed proportion of beats get through, often one in two, giving a QRS (and hence heart) rate of 150 b/min. The right atrial circuit is usually of such a length that 300 circuits occur per minute. 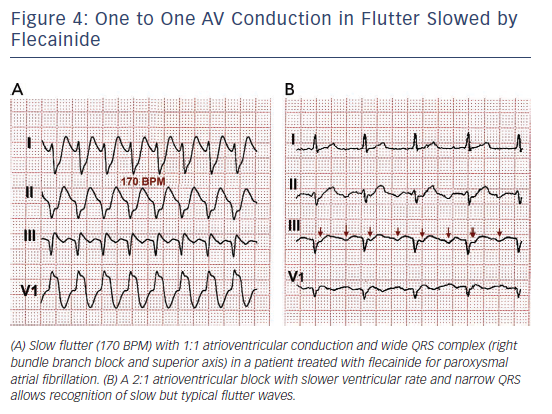
Occasionally the P waves in lead V1 are not well developed. P wave activity is often reasonably well seen in lead V1, when it is predominantly positive. The ‘sawtooth’ baseline typically has a slow downstroke and a rapid upstroke. 44.1a– d) and results in a highly characteristic ECG appearance, with continual electrical activity best seen in the inferior leads. It is due to a macro re-entrant circuit in the right atrium ( Fig. It is important to distinguish atypical flutter from typical flutter because this tells you something about how easy the rhythm will be to control (with meds) or treat (in EP lab).Atrial flutter is a common arrhythmia, especially in men (perhaps as they have larger hearts) ( Table 44.1). These can have all kinds of different A wave patterns and rates. For instance, there can be a circuit that relies on the tricuspid opening and a scar or one that relies on the mitral opening and an area previously treated with ablation for afib (endless possibilities). "Atypical flutter" is any other circuit in the heart that depolarization can travel along in a self-sustaining way. In clinical practice, the distinction of whether depolarization is clockwise or counterclockwise is not very relevant (does not affect management at all) so we usually don't mention it on ECGs, etc. The depolarization can be traveling either clockwise or counterclockwise in "typical flutter" (you can even have both, at different times, in the same patient). If someone has had surgery or ablation, the rules kind of go out the window.Īs others have said, "typical flutter" is anatomically defined: it is flutter that relies on the CTI as part of its circuit. The rate can be anywhere from 200 bpm (esp if there’s a significant degree of RA dilation) up to a little over 300 bpm. If it doesn’t look typical it is still probably typical. The ECG appearance is primarily due to the vector of activation along the lateral wall of the right atrium as seen on the inferior leads and in lead V1.įrom a practical standpoint: Patients without prior surgery or ablation, if it looks typical it very likely is typical. By this time the tissue is able to conduct and then you have a beat of atrial flutter. The enters the CTI from left to right, blocks, then travels around the tricuspid valve until it reaches the CTI from the other direction. This can be using zones of slow conduction from prior surgery, ablation, or areas of diseased atrial myocardium.Ĭounterclockwise (CCW) flutter is most common because there is a higher likelihood of PACs initiating the arrhythmia from the atria to the anatomical left of the CTI. The most accurate description of an atypical flutter is a macro reentrant atrial tachycardia. The nomenclature is really unfortunate, as flutter is a description of symptoms. 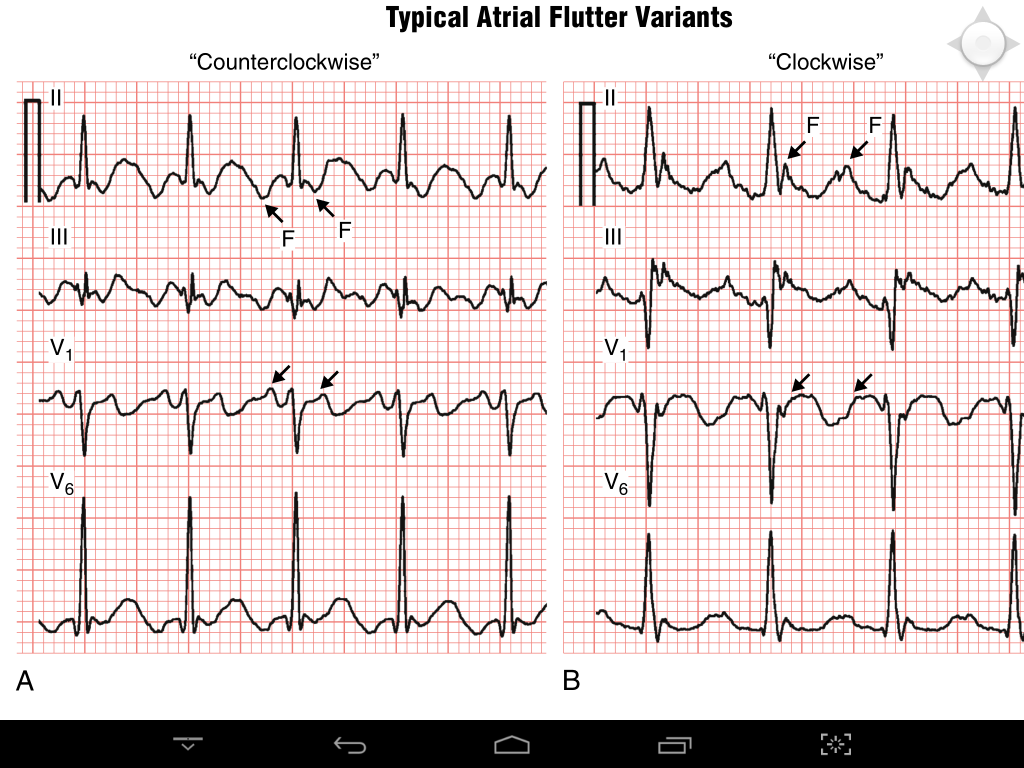 
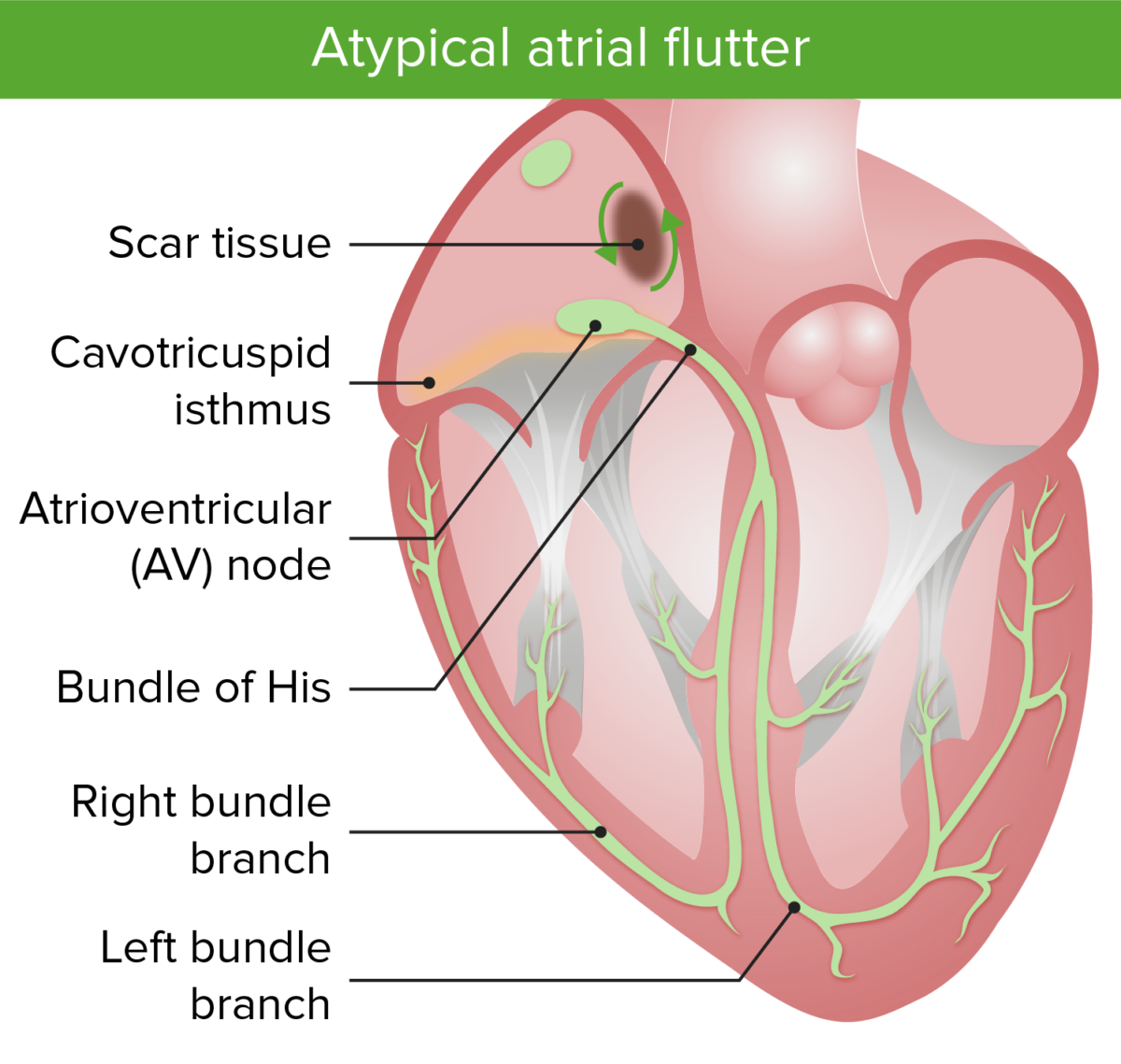
As someone else said, the only difference is whether the arrhythmia circuit utilizes the cavotricuspid isthmus (CTI) in typical flutter, or something else in atypical flutter. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
